In 2015, a team of researchers at the Weizmann Institute of Science ran a study that should have changed the way the entire world thinks about diet advice. They gave 800 participants identical meals and measured their glucose responses. The expectation was that similar meals would produce similar results.
They did not.
The same standardized meal caused a glucose spike of 40 mg/dL in one person and 120 mg/dL in another. The range of responses was enormous and could not be explained by body weight, age, or obvious health markers alone.
The Study That Broke the "Good Food, Bad Food" Myth
The research, published in the journal Cell by Zeevi and colleagues, tracked 800 people over a week, collecting nearly 47,000 meal measurements. Each participant ate several standardized meals so the researchers could compare apples to apples - same food, same portion, different people.
The key findings:
- Individual variation in glucose response was larger than the variation between foods. In other words, the difference between how two people respond to the same bread was bigger than the difference between bread and chocolate for many individuals.
- Traditional glycemic index (GI) rankings were poor predictors of individual response. A food labelled "low GI" could cause a large spike in some participants, while a "high GI" food caused minimal response in others.
- Gut microbiome composition was one of the strongest predictors of individual glucose responses, along with factors like insulin sensitivity, recent meal history, and time of day.
The implication is direct: generic dietary advice - "eat low-GI foods," "avoid white rice," "choose whole grains" - is a reasonable starting point, but it fails many individuals. Your body does not read nutrition labels. It responds based on your unique biology.
Why Individual Variation Matters So Much
This is not an academic distinction. For someone managing prediabetes, the practical difference is significant.
Consider two people, both with prediabetes, both eating idli for breakfast:
- Person A spikes to 150 mg/dL (a modest, well-controlled response)
- Person B spikes to 195 mg/dL (a response in the diabetic range)
If both followed generic advice that says "idli is moderate GI, it should be fine," Person B would unknowingly eat a problematic food every morning. Only by testing their own glucose response could Person B discover that idli is not, in fact, a safe choice for their body - and perhaps switch to wheat dosa or roti with dal, which might produce a much better response.
The Zeevi study also found that the time of day dramatically affects glucose response. The same meal eaten at breakfast might produce a different spike than at lunch, because morning insulin resistance (the dawn phenomenon) amplifies carbohydrate impact. This means your personal "safe foods" might depend not just on the food itself, but on when you eat it.
What Drives Your Unique Response
Research has identified several factors that explain why glucose responses are so individual:
Gut microbiome: The composition of bacteria in your digestive system affects how quickly carbohydrates are broken down and absorbed. Two people with different microbiome profiles can process the same food at very different rates.
Insulin sensitivity: How effectively your cells respond to insulin varies widely between individuals and even within the same individual at different times of day. Morning insulin sensitivity is typically 30% lower than afternoon sensitivity.
Prior meal effects: What you ate at your last meal influences how your body handles the next one. A low-GI dinner can improve your glucose response at breakfast the next morning by 20-40 mg/dL (the "second meal effect").
Gastric emptying rate: How quickly your stomach releases food into the small intestine affects the speed of glucose absorption. This varies significantly between individuals.
Physical activity: Recent exercise improves glucose uptake for 12-24 hours after the activity. Two people eating the same meal will have different responses if one exercised that morning and the other did not.
The Only Way to Know Is to Test
This is the core argument for personal glucose experimentation. Population studies tell you what works on average. Your glucometer tells you what works for you.
The methodology is straightforward. It is called an N-of-1 trial, a concept formalized by Guyatt and colleagues in the New England Journal of Medicine in 1986. The idea is simple: you are your own control group. Test a food under controlled conditions, repeat it at least 3 times, and your average response is a reliable indicator of how your body handles that food.
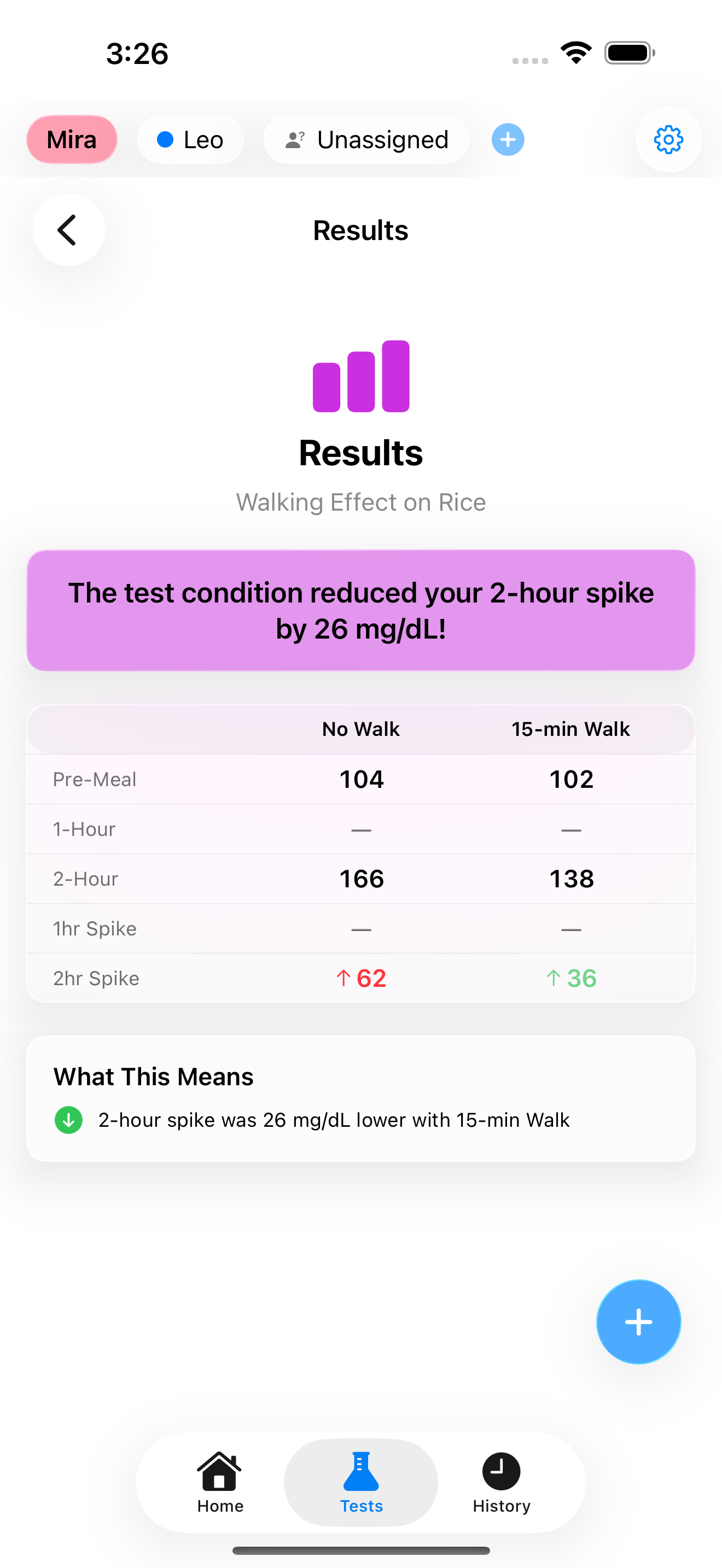
How Prick Helps You Find Your Own Answers
Prick includes 7 experiment templates designed to help you test the variables that matter most:
- Walking Effect: Same meal with and without a post-meal walk
- Carb Order: Rice-first vs. vegetables-and-dal-first
- Portion Size: Finding the threshold where your glucose stays in range
- New Food: Testing an unfamiliar food against a known baseline
- Fiber Pairing: Plain carbs vs. carbs with added fibre and protein
- Consistency: Repeating the same meal to check how reliably your body responds
- Custom: Design your own experiment with any two conditions
Each template guides you step by step: when to take your baseline reading, when to eat, when to measure your post-meal response. The app tracks your paired results and shows the comparison so you can see, in your own data, what actually works.
Generic advice says "eat less rice." Your experiment might show that 1 cup of rice with dal and vegetables keeps you under 140 mg/dL, while 1 cup of rice alone pushes you to 185. That is the difference between deprivation and informed eating.
Based on: Zeevi et al. (2015), Personalized Nutrition by Prediction of Glycemic Responses; Guyatt et al. (1986), N-of-1 Trials; Individual Variation Research
View full citations
- Zeevi D, et al. "Personalized Nutrition by Prediction of Glycemic Responses." Cell. 2015;163(5):1079-1094. https://doi.org/10.1016/j.cell.2015.11.001
- Guyatt G, et al. "Determining Optimal Therapy - Randomized Trials in Individual Patients." New England Journal of Medicine. 1986;314(14):889-892. https://doi.org/10.1056/NEJM198604033141406
- Mendes-Soares H, et al. "Assessment of a Personalized Approach to Predicting Postprandial Glycemic Responses to Food Among Individuals Without Diabetes." JAMA Network Open. 2019;2(2):e188102. https://doi.org/10.1001/jamanetworkopen.2018.8102