You ate a reasonable dinner. You skipped the late-night snack. You even went for a short walk. And yet your fasting glucose this morning is 125 mg/dL. What happened?
For many people with prediabetes, the answer has nothing to do with food. It has to do with what happened between dinner and your morning reading: how well you slept, how stressed you were during the day, and whether your body's hormonal rhythms operated normally overnight.
Sleep and stress are the invisible factors in glucose control. They do not show up on your plate, but they show up in your numbers.
The Sleep-Glucose Connection
Sleep is not passive rest. It is an active metabolic process during which your body repairs insulin receptors, regulates cortisol and growth hormone, and processes the day's glucose load. When sleep is disrupted, every part of this system suffers.
The research quantifies this precisely:
- 8 hours of sleep: Fasting glucose typically 95-105 mg/dL for someone in the prediabetic range
- 6-7 hours of sleep: Fasting glucose rises to approximately 105-115 mg/dL
- 5 hours of sleep: Fasting glucose climbs to 115-130 mg/dL - an increase of 20-25 mg/dL from baseline
- 4 hours of sleep: Fasting glucose can reach 125-145 mg/dL, with significant impairment in insulin sensitivity
That means one bad night of sleep can elevate your fasting reading by 10-20 mg/dL - the same impact as a poor meal choice. And unlike a meal, you cannot compensate for lost sleep with a post-dinner walk.
But it is not just the number of hours. The timing and consistency of sleep matter independently.
Late bedtime matters. Going to bed at midnight instead of 10 PM - even if you sleep the same total number of hours - adds 10-20 mg/dL to fasting glucose. This is due to circadian misalignment: your body's internal clock expects certain metabolic processes to happen at specific times. Sleeping late disrupts this programming.
Irregular sleep schedule matters. Research shows that inconsistency in sleep timing raises HbA1c independently of total hours. If you go to bed at 10 PM on weekdays and 1 AM on weekends, your glucose control suffers even on the days you sleep well.
Sleep quality matters. Fragmented sleep - waking multiple times through the night - impairs insulin sensitivity more than slightly shorter but continuous sleep. Deep, uninterrupted sleep is when the most repair happens.
The Stress-Cortisol Pathway
When you are stressed, your body releases cortisol. This is a survival mechanism: cortisol signals the liver to release glucose into the bloodstream, preparing you for physical action. In evolutionary terms, stress meant physical danger, and extra blood glucose meant extra energy to fight or run.
The problem is that modern stress is rarely physical. Work deadlines, family worry, financial pressure, health anxiety - none of these require extra blood glucose. But your body releases it anyway. Cortisol also reduces insulin production and makes your cells less responsive to the insulin you do produce. The result: blood glucose rises without you eating anything.
Research from Ohio State University found that people with type 2 diabetes who had dysregulated cortisol patterns - where cortisol stays elevated throughout the day instead of following the normal morning-peak-to-evening-decline pattern - had significantly worse glucose control.
The impact of stress on glucose is not trivial:
- A high-stress day can raise glucose by 15-30 mg/dL across all readings
- Chronic stress worsens HbA1c by 0.2-0.4% - comparable to modest dietary changes
- The combination of stress and poor sleep has a synergistic (not just additive) effect on glucose
This means that a stressed, sleep-deprived week can raise your average glucose as much as abandoning dietary improvements entirely. If you have been eating well but your numbers are not improving, stress and sleep deserve serious attention.
The Dawn Phenomenon: Why Morning Readings Are Special
There is a specific hormonal event that makes morning glucose readings uniquely sensitive to sleep and stress: the dawn phenomenon.
Between 3 AM and 8 AM, your body releases a surge of hormones - cortisol, growth hormone, and glucagon - that prepare you to wake up. In a person without diabetes, the pancreas compensates by releasing extra insulin, and glucose stays stable. In someone with prediabetes or diabetes, the insulin response is inadequate, and fasting glucose rises.
The dawn phenomenon occurs in over 50% of people with diabetes and can raise glucose by 10-40 mg/dL by morning. It is worsened by poor sleep, stress, and late-night eating. It is improved by consistent sleep timing, adequate sleep duration, and an appropriate evening meal.
This is why fasting glucose is such a revealing measurement. It does not just tell you what you ate last night. It tells you the cumulative state of your hormonal regulation, sleep quality, stress level, and metabolic health.
Practical Steps for Better Morning Numbers
Understanding the science is useful. But practical changes are what move the numbers.
Sleep hygiene that matters for glucose:
- Aim for 7-8 hours per night, at a consistent time. Going to bed by 10 PM is associated with better fasting glucose than the same hours starting at midnight.
- Keep your sleep schedule consistent across weekdays and weekends. A 2-hour shift in bedtime on weekends creates the same metabolic disruption as partial sleep loss.
- Avoid large meals within 2-3 hours of bedtime. Digesting a heavy meal during sleep raises blood glucose overnight and worsens the dawn phenomenon.
- Reduce screen time in the hour before bed. Blue light from phones and televisions suppresses melatonin and delays sleep onset.
Stress management that measurably affects glucose:
- Physical activity during the day - even a 15-minute walk - improves both sleep quality and cortisol regulation. This creates a positive feedback loop: better activity leads to better sleep leads to better glucose.
- Relaxation practices like yoga, pranayama, or meditation have been shown to lower cortisol and improve glucose control. For someone in Bangalore, a morning yoga routine is both culturally familiar and metabolically beneficial.
- Recognising stress as a glucose factor is itself valuable. When you see an elevated fasting reading after a stressful day, knowing the mechanism prevents the frustration of thinking your diet has failed.
How Prick Helps You See the Pattern
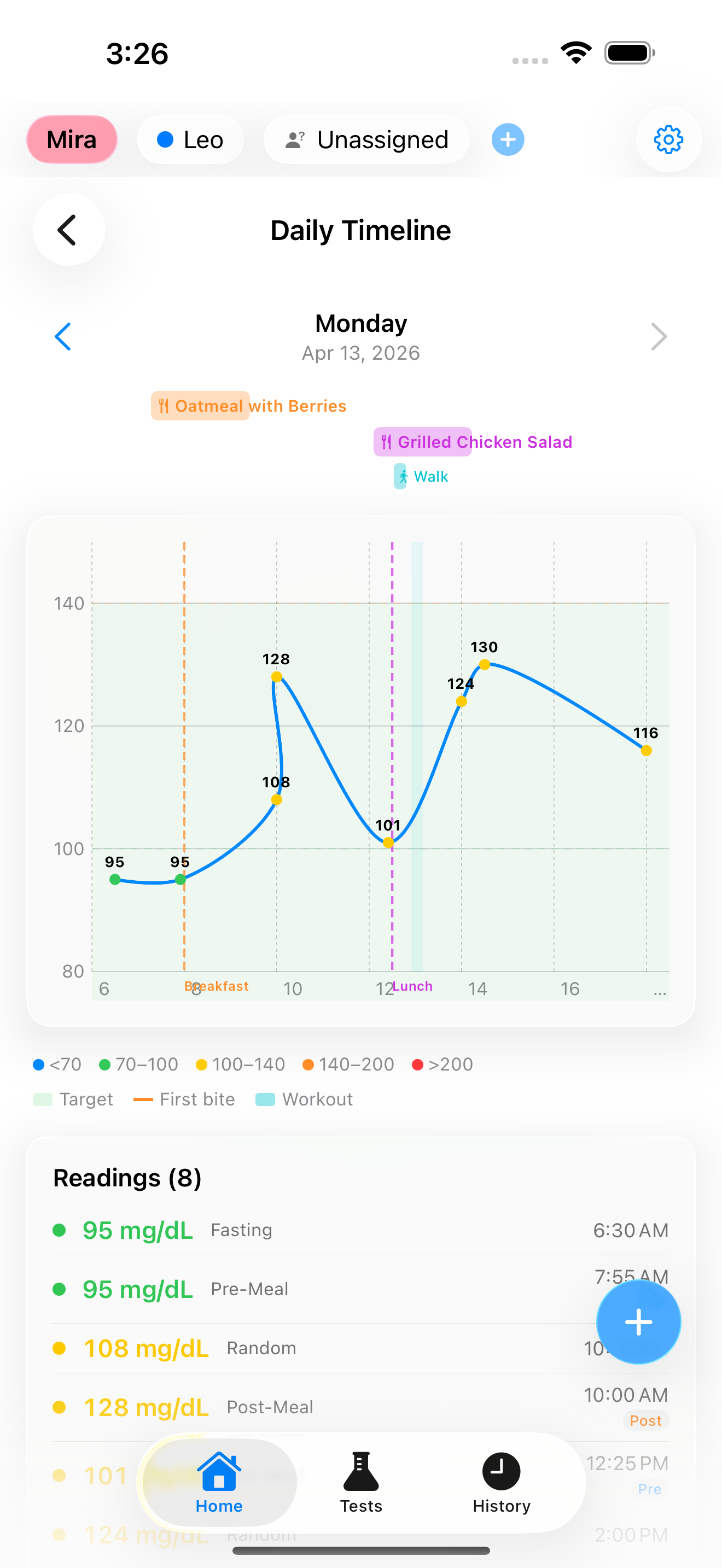
Prick's notes field lets you record context alongside every reading. When you log "poor sleep" or "stressful day" alongside your fasting glucose, a pattern emerges over weeks that is impossible to see from a single reading.
The daily timeline view shows all your readings for a day alongside their context notes. Over time, you may notice that your fasting glucose on mornings after 7+ hours of sleep is consistently 10-15 mg/dL lower than after short nights. That is your personal data confirming what the research shows at the population level.
If your fasting glucose is stubbornly elevated and you cannot find a dietary explanation, look at your sleep and stress patterns first. The answer is often there, hidden in the hours you were not thinking about glucose at all.
The Key Takeaway
Food is not the only thing that affects your glucose. Sleep duration, sleep timing, sleep consistency, daily stress, and the dawn phenomenon all contribute to your morning number. A person who eats perfectly but sleeps poorly and lives under chronic stress will see higher glucose than a person with a moderate diet, good sleep, and low stress.
Managing prediabetes is about managing your whole life, not just your plate. The most powerful morning glucose intervention might not be what you eat for dinner. It might be going to bed an hour earlier.
Based on: Spiegel K et al. (1999), sleep and metabolic function; Reutrakul S & Van Cauter E (2018), sleep and diabetes risk; OSU cortisol-glucose study; circadian rhythm research
View full citations
- Spiegel K, et al. "Impact of Sleep Debt on Metabolic and Endocrine Function." The Lancet. 1999;354(9188):1435-1439. https://doi.org/10.1016/S0140-6736(99)01376-8
- Reutrakul S, Van Cauter E. "Sleep Influences on Obesity, Insulin Resistance, and Risk of Type 2 Diabetes." Metabolism. 2018;84:56-66. https://doi.org/10.1016/j.metabol.2018.02.010
- Hackett RA, Steptoe A. "Type 2 Diabetes Mellitus and Psychological Stress - a Modifiable Risk Factor." Nature Reviews Endocrinology. 2017;13(9):547-560. https://doi.org/10.1038/nrendo.2017.64
- Leproult R, et al. "Circadian Misalignment Augments Markers of Insulin Resistance and Inflammation, Independently of Sleep Loss." Diabetes. 2014;63(6):1860-1869. https://doi.org/10.2337/db13-1546