Important: This article is educational. Never change when you take your medication without first discussing it with your prescribing doctor. Medication timing affects both effectiveness and side effects, and the right approach depends on your specific health situation.
If you have been prescribed metformin for prediabetes or type 2 diabetes, you were almost certainly told to take it "with food." This is standard advice, and it is given for a good reason: metformin taken on an empty stomach can cause nausea and stomach upset. Taking it with a meal reduces these side effects.
But recent research suggests that the timing of metformin relative to meals may meaningfully affect how well it works. And the standard advice of "take with food" may not be optimal for everyone.
What the Research Shows
Metformin works primarily by reducing the liver's glucose output and improving insulin sensitivity. But it also acts in the gut, affecting how glucose from food is absorbed. This gut mechanism is why timing matters: metformin needs to be present in the digestive system when food arrives.
Studies comparing different timing windows have found measurable differences:
- 30-60 minutes before a meal: Approximately 20-30 mg/dL reduction in both fasting glucose and post-meal glucose
- With the meal (standard recommendation): Approximately 15-20 mg/dL reduction
- 60+ minutes after a meal: Only approximately 5-10 mg/dL reduction
The difference between taking metformin 30 minutes before a meal versus with a meal is 5-10 mg/dL. That may sound modest, but over months and years, it translates to a meaningful difference in average glucose and estimated HbA1c.
The mechanism behind this difference appears to be related to GLP-1, a hormone that helps regulate blood sugar. When metformin is already in the gut before food arrives, it enhances the GLP-1 response more effectively than when it arrives at the same time as the food.
Extended-Release Metformin
Many people take the extended-release (ER or XR) form of metformin, which is designed to dissolve slowly and provide steady medication levels throughout the day. Extended-release metformin is typically taken once daily with the evening meal.
The timing research primarily studied immediate-release metformin (the standard form taken 2-3 times daily). The principles likely apply to extended-release formulations as well, but the timing window is less critical because the medication releases gradually. If you take extended-release metformin, your doctor's current timing recommendation is likely appropriate.
Why "Take With Food" Became Standard
The "take with food" instruction exists because metformin's most common side effects are gastrointestinal: nausea, diarrhea, stomach cramping, and bloating. These side effects are significantly reduced when the medication is taken alongside food, which buffers the drug's irritation of the stomach lining.
For many people, especially those just starting metformin, taking it with food is the right approach. The priority during the first weeks is tolerability. If you cannot tolerate the medication, the timing advantage of taking it earlier is irrelevant.
The research finding is that once you tolerate metformin well - which most people do after the first 2-4 weeks - it may be worth discussing the timing with your doctor. Moving the dose from "with breakfast" to "30 minutes before breakfast" is a simple change that some people find produces noticeably better post-meal readings.
What This Means for You
This is not a recommendation to change your medication timing on your own. It is information to bring to your next doctor's appointment.
Here is a practical way to approach the conversation:
If you are currently taking metformin with meals and tolerating it well, ask your doctor: "I have read that taking metformin 30 minutes before meals might be more effective. Is that worth trying for me?"
If you experience GI side effects from metformin, the current timing with food is almost certainly the right approach for you. The marginal glucose benefit of earlier timing is not worth increased nausea or stomach upset.
If your glucose readings are not improving as expected despite taking metformin as prescribed, timing is one of several variables worth discussing with your doctor. Others include dose adjustment, dietary changes, and activity level.
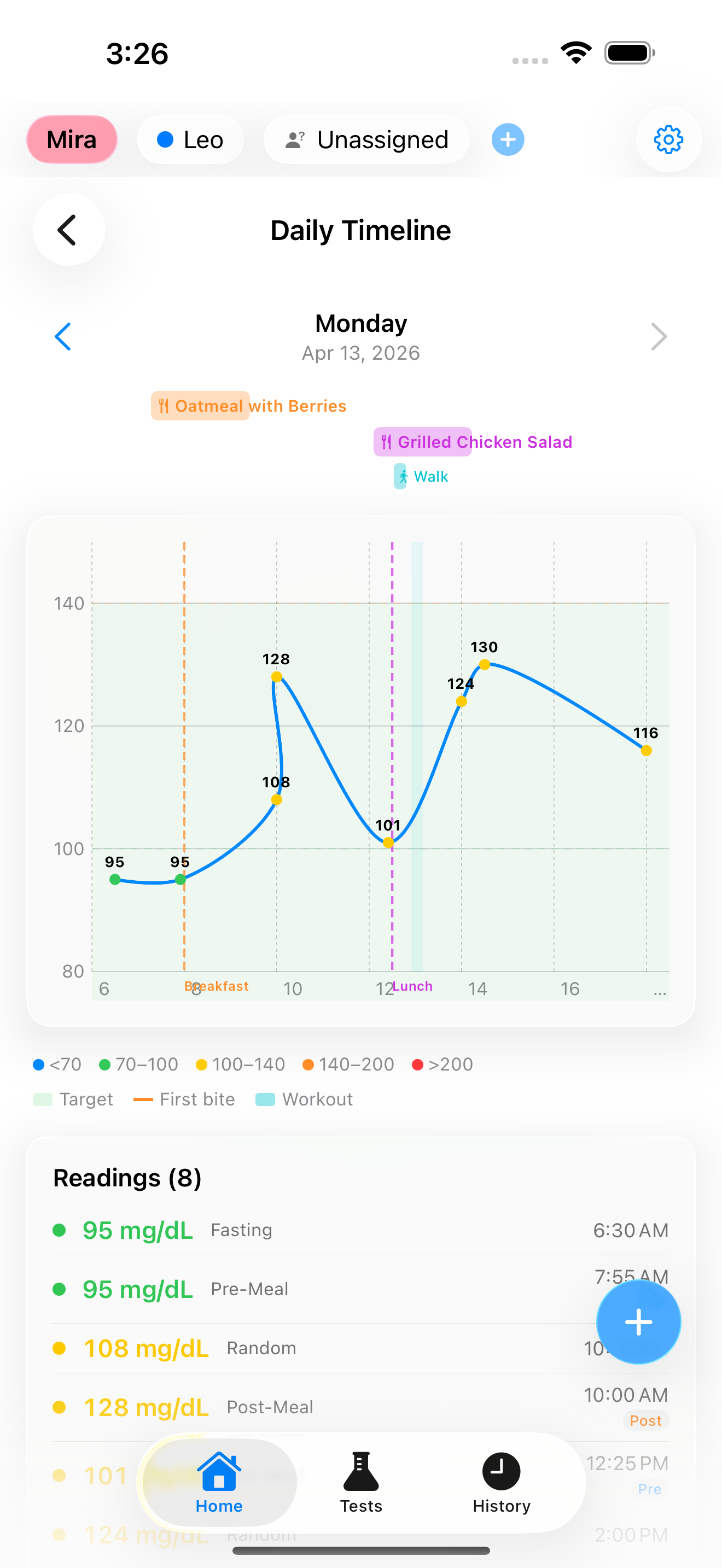
How Prick Helps You Track Medication Impact
Prick's daily timeline shows all your glucose readings across the day alongside your meals and notes. If you and your doctor decide to try adjusting your medication timing, you can log the timing change in the notes field and observe the effect on your post-meal readings over the following weeks.
The Medication Timing experiment template in Prick is designed for exactly this kind of structured comparison. With your doctor's approval, you can run a paired test: one week taking metformin at your current time, one week at the adjusted time, same meals. The app shows the comparison side by side.
This kind of personal data is valuable for your doctor too. Rather than describing your experience verbally, you can show them a chart of your post-meal readings before and after the timing change. Doctors make better decisions with better data.
Beyond Timing: Metformin in Context
Metformin is an effective medication, but it is not a replacement for lifestyle changes. The Diabetes Prevention Program showed that lifestyle intervention (diet plus exercise) reduced diabetes risk by 58%, while metformin alone achieved 31%. The combination of both is most effective.
Think of metformin as one tool in a larger strategy. Optimising its timing may improve its contribution by 5-10 mg/dL. Adding a post-meal walk improves glucose by 20-30 mg/dL. Eating dal and vegetables before rice reduces the spike by 25-40 mg/dL. Improving sleep quality lowers fasting glucose by 10-20 mg/dL.
All of these interventions are additive. Medication timing, meal composition, physical activity, and sleep each contribute. The most effective approach combines all of them.
The Key Takeaway
Research suggests that metformin taken 30-60 minutes before a meal may be more effective than taking it with a meal, primarily through enhanced GLP-1 response. But this is a conversation to have with your doctor, not a change to make on your own. If you tolerate your medication well and your readings are not where you want them, timing is a variable worth discussing at your next appointment.
Bring your glucose data from Prick. Show your doctor your post-meal patterns. Let the conversation be guided by your numbers, not guesswork.
Based on: Metformin pharmacokinetics research; Foretz M et al. (2014), metformin mechanisms; ADA Standards of Care 2023; DPP study comparison
View full citations
- Foretz M, et al. "Metformin: From Mechanisms of Action to Therapies." Cell Metabolism. 2014;20(6):953-966. https://doi.org/10.1016/j.cmet.2014.09.018
- Graham GG, et al. "Clinical Pharmacokinetics of Metformin." Clinical Pharmacokinetics. 2011;50(2):81-98. https://doi.org/10.2165/11534750-000000000-00000
- American Diabetes Association. "Pharmacologic Approaches to Glycemic Treatment: Standards of Medical Care in Diabetes - 2023." Diabetes Care. 2023;46(Suppl 1). https://doi.org/10.2337/dc23-S009
- Knowler WC, et al. "Reduction in the Incidence of Type 2 Diabetes with Lifestyle Intervention or Metformin." New England Journal of Medicine. 2002;346(6):393-403. https://doi.org/10.1056/NEJMoa012512